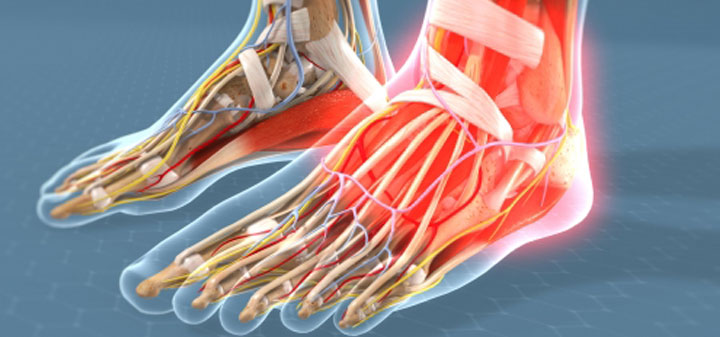
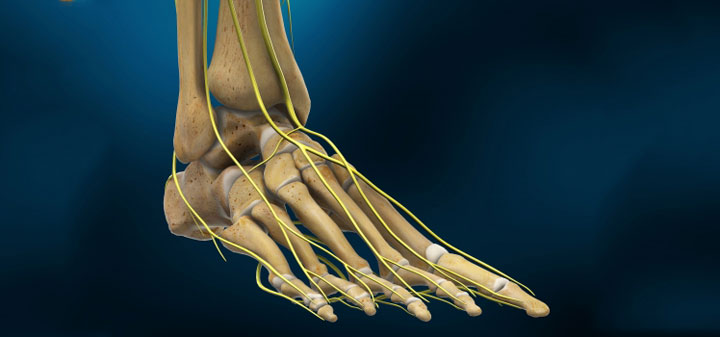
What Causes the Feet to go Flat?
 Flatfoot is a term used to describe a collapsed arch. Medically, the term is pes planovalgus (for a flattened foot that is pushed outwards). There are varying degrees of ‘flatness.’ While some flat feet are not problematic at all, there are those that are painful and can cause significant discomfort and have a big impact on one’s ability to be active. There are two kinds of flat feet – flexible (mobile) or rigid (stiff). A flexible flatfoot is one where the foot retains motion. This type is considered to be hypermobile and the arch is able to be recreated when there is no weight on the foot. A flexible flatfoot is a very common form of flatfoot that usually originates in childhood and lasts throughout adulthood, typically worsening without treatment. The deformity in flexible flatfoot involves a mild, gradual collapse of the foot’s arch, and almost always occurs in both feet. In contrast, a rigid flatfoot is ‘stuck’ in the flat position regardless of whether or not there is pressure placed on the foot. The successful treatment of flexible or rigid flat feet depends on an accurate diagnosis, early treatment and in some cases proper procedure selection.
Flatfoot is a term used to describe a collapsed arch. Medically, the term is pes planovalgus (for a flattened foot that is pushed outwards). There are varying degrees of ‘flatness.’ While some flat feet are not problematic at all, there are those that are painful and can cause significant discomfort and have a big impact on one’s ability to be active. There are two kinds of flat feet – flexible (mobile) or rigid (stiff). A flexible flatfoot is one where the foot retains motion. This type is considered to be hypermobile and the arch is able to be recreated when there is no weight on the foot. A flexible flatfoot is a very common form of flatfoot that usually originates in childhood and lasts throughout adulthood, typically worsening without treatment. The deformity in flexible flatfoot involves a mild, gradual collapse of the foot’s arch, and almost always occurs in both feet. In contrast, a rigid flatfoot is ‘stuck’ in the flat position regardless of whether or not there is pressure placed on the foot. The successful treatment of flexible or rigid flat feet depends on an accurate diagnosis, early treatment and in some cases proper procedure selection.
What are the Symptoms of Flat Feet?
Flat feet can exhibit a variety of symptoms – from mild to severe. The severity of the flattening of the arch/foot does not always correlate with the extent of symptoms. Patients may complain of arch pain and heel pain. Commonly there is pain on the outside of the foot – where the foot meets the ankle as the collapse foot abuts against the ankle. Muscle cramps within the foot, and onto the leg (shin splints) may occur. Patients may also experience lower back pain or leg fatigue.
In general, patients have pain with activity such as walking or running. The pain may be deep and focal to a generalized widespread achy feeling. Patients also complain of having a hard time finding the “right” shoe, uneven wear of their shoe, and the foot rolling inward when they walk causing a collapsing of the shoe. When seen in children, pain is not a typical complaint, but fatigue is. If your child is not able to keep up with their peers on the playground or easily gets tired when doing a lot of walking, this may be an indication that their flat feet are an issue as a fallen arch is very inefficient at walking and running and can drain energy quickly leading to decreased stamina. Some of these kids become “couch potatoes” as they will eventually favor activities that are not physical. This can lead to more problems later in life even though pain may not be an initial symptom.
Causes of Flat Feet
There are a variety of causes of flat feet. Flat feet can be genetic, acquired and develop over time. Young children and teens can have flattened feet. Injury can lead to flat feet. Tendon problems, and arthritis can lead to flat feet. Rigidly flat feet may occur from a condition called tarsal coalition, where the bones in the back of the foot are genetically fused or locked together. A detailed physical exam and x-rays can help to diagnosis this, but it is usually best seen with either an MRI or CT scan. Flat feet are also associated with congenitally tight Achilles tendons or calf muscles and develop as the body tries to compensate for this by causing the foot to become hypermobile in the arch, thus flattening it. While a number of articles have been written in an attempt to identify the cause of flat feet, most agree that it is multi-factorial meaning that there is more than one cause.
Diagnosing Flexible Flatfoot
 If your feet are causing you problems, visit your foot and ankle specialist for an exam. Dr. Perler will take a close look at the structure of your feet and examine how your foot moves and changes shape while sitting, standing, or taking steps. An X-ray can be helpful to understand the severity of the condition. If a tendon or ligament tear is thought to be possible, an MRI may be ordered. In some cases where it Is felt that your flatfoot is not flexible, a CT scan may be helpful in ruling out the joining of two bones that could lead to a reduction of motion (congenital tarsal coalition).
If your feet are causing you problems, visit your foot and ankle specialist for an exam. Dr. Perler will take a close look at the structure of your feet and examine how your foot moves and changes shape while sitting, standing, or taking steps. An X-ray can be helpful to understand the severity of the condition. If a tendon or ligament tear is thought to be possible, an MRI may be ordered. In some cases where it Is felt that your flatfoot is not flexible, a CT scan may be helpful in ruling out the joining of two bones that could lead to a reduction of motion (congenital tarsal coalition).
Treatments
Depending on your overall health, symptoms, and severity of the flat foot, the condition may betreated conservatively and/or with surgery. Non-surgical treatments for flat feet are centered at decreasing and/or resolving the symptoms (pain).

Simple Treatments Patients Can Do:
- Wear proper supportive shoes
- Use an arch support (over the counter or custom)
- Wear shoes with a wide toe box
- Modify your activities
- Lose weight
- Stretch the calf/Achilles tendon
- Strengthen their arch muscles with an at-home exercise program
- Wear shoes with cushion
Non-surgical treatments Dr. Perler may add:
- Prescribe an oral anti-inflammatory medication
Anti-inflammatory medication is useful to significantly reduce pain and inflammation. This can be in the form of an oral steroid, an oral NSAID (like Ibuprofen or Mobic), a prescriptive topical cream or patch, or a custom topical compound medication.
- Prescribe physical therapy
A physical therapist may perform ultrasound and other techniques to reduce inflammation. You will also be instructed on how to stretch your foot and leg properly. Keeping the joint mobile may preserve function. Strengthening weak foot and leg musculature can help prevent further collapse.
- Prescribe custom foot orthotics
A custom foot orthotic is a doctor prescribed arch support that is made directly from a casting (mold) of your feet, and theoretically should provide superior support compared to shoe insert that you would purchase from a pharmacy. In the case of flat feet, specific modifications can be made to the orthotic device to strategically balance the foot.
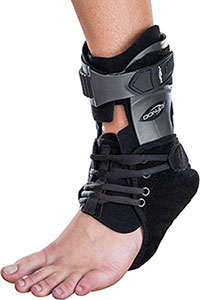
- Prescribe a custom ankle-foot orthoses
A custom ankle-foot orthotic (AFO) is a doctor prescribed molded arch and lower leg support that stabilizes both the foot and ankle. This is used when the flat foot is significant and provides more support than the simple foot-only insert.
- Give cortisone injection
An articular (into the joint) cortisone injection is a powerful anti-inflammatory medication that is used to rapidly reduce the pain associated with inflammation. Cortisone shots can be extremely effective in alleviating symptoms of flat feet, but will not correct the structure. Dr. Perler does not recommend cortisone injections by tendons as they can weaken the tendon and are related to a higher incidence of tendon rupture.

- Discuss Regenerative Medicine Injection Therapy
In certain cases where there is advancing tendon inflammation and degeneration that doesn’t respond to a traditional anti-inflammatory approach, an injection using advanced biologics such as a platelet rich plasma injection or an amniotic tissue matrix injection may be helpful. This is a very exciting type of therapy that is aimed at patients being able to heal their own damaged tissue with aided stimulation from outside growth factors injected directly into the faulty tendon.
FlatFoot Surgery
In the event that conservative treatments are not capable of properly addressing the symptoms associated with your flat foot, more drastic measures may need to be taken to get you back on track with your healing process. In certain cases, Dr. Perler may recommend surgical intervention to address your needs. Surgery for flat feet is separated into three kinds: soft tissue procedures, bone cuts (osteotomies), and bone fusions. Depending on the severity of the flat foot, a person’s age, and whether or not the foot is stiff determines just how the foot can be fixed. In most cases a combination of procedures are performed.

With flexible flat feet, surgery is geared at maintaining the motion of the foot and recreating the arch. Commonly this may involve tendon repairs along the inside of the foot to reinforce the main tendon that lifts the arch. Also, if the Achilles tendon is found to be overly tight, Dr. Perler will routinely recommend a calf muscle lengthening. When the arch collapse is significant, boney procedures are included to physically rebuild the arch, and realign both the heel and foot. The presence of bunions with flat feet is often contributing to the collapse and in most situations requires correction.
With rigid flat feet, surgery is focused on restoring the shape of the foot through procedures that eliminate motion (fusion). In this case, motion does not exist preoperatively, so realigning the foot is of utmost importance. The exception, are rigid flat feet due to tarsal coalition (a fused segment of bone) often seen in children located in the back of the foot where freeing the blockage can restore more normal function.
What Are the Goals of Flatfoot Surgical Correction?
The goal of surgical correction is to improve both the function and alignment of the foot. This allows for more normal pressures during standing and walking. Proper correction of the flatfoot deformity can often help to improve pain, walking ability, improve muscular fatigue, and return you to a more active lifestyle.
When Should I Avoid Surgery?
Patients who have diabetes or take oral steroids should be evaluated by their primary care physician. These conditions may prevent you from being able to safely have surgery. Significantly obese patients and smokers are at higher risk for blood clots and wound problems. Full recovery from flatfoot surgery can take up to a year. Patients who are unable or unwilling to complete this process are not ideal candidates and should avoid having this type of surgery.
Surgical Techniques
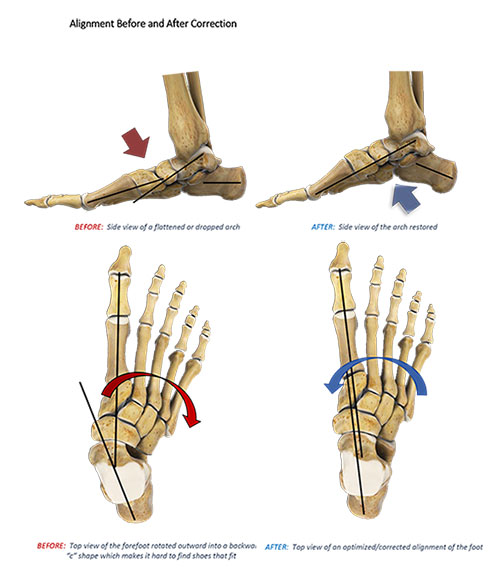
General Details of Procedure
In feet that where the deformity is significant, a combination of surgical procedures can be used to realign and reconstruct the flatfoot. Generally, these procedures can be separated into those that correct deformities of the bones and those that repair ligaments and tendons. After a though workup, Dr. Perler will help you choose the proper combination of procedures to optimize the correction of your flatfoot.
Surgery of the foot can be performed under regional anesthesia, which is numbing the foot and ankle with a nerve or spinal block, or general anesthesia, which may require a breathing tube. A nerve block is often placed behind the knee to reduce pain after surgery. It is usually a “same day” procedure meaning you can return home the day of the procedure.
Soft Tissue Repairs
Tendon Transfers & Augmentations (Kidner Procedure)
With flat feet, there is a tendon on the inside of the foot than can often become weakened, injured, split and/or ruptured. This tendon, called the posterior tibial tendon, is the main arch supporting tendon. Damage to this tendon can cause collapse of the arch, which is often the main cause of an adult onset flatfoot deformity. In mild cases, where the tendon is thickened but not frayed or tone, a minimal incision approach can be taken with ultrasound based debridement and the injection of amniotic tissue. This approach fits under the category of regenerative medicine where the tendon is aerated, seeded, and fertilized to promote new tissue growth using your body’s own ability to heal.
When the tibialis posterior tendon disease is more advanced, such as tendon splits, the posterior tibial tendon can be repaired or grafted with either collagen or a synthetic material to restore its strength. Acute ruptures of the tendon can be primarily repaired. Often the posterior tibial tendon is augmented with a tendon transfer of an adjacent tendon to provide both strength and continuity. Usually the tendon that bends the little toes can be transferred (rerouted) to help support the arch.
Some people have genetically inefficient tendon which may be the case in younger people. In the posterior tibial tendon advancement (Kidner Procedure) the tendon is often advanced or re-tensioned to restore its function and any excessive bone is removed. In most flat foot surgery a tendon repair or augmentation is often combined with other boney procedures to restore structure and balance to the foot.
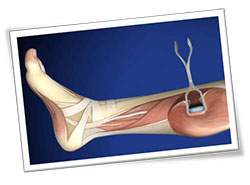
Achilles Tendon/Calf Muscle Lengthening
The flatfoot condition is often associated with tightness of the Achilles tendon. This may be congenital (born with it) or acquired over time. This can be treated using a lengthening procedure (intramuscular gastrocnemius recession) to stretch the muscle fibers of the calf
Joint Spacers (Artheroesis Procedures)
A procedure that involves placing a metallic implant (most commonly) at the junction where the foot meets the ankle. This device causes the physical blockade that prevent the collapse. It is a procedure that is only indicated for mobile feet, and should not be used with rigid flat feet. Dr. Perler typically only uses this device as a temporary “rest” for a diseased tibialis posterior tendon that has been repaired or debrided or in individuals who cannot go through the more extensive surgical corrections.
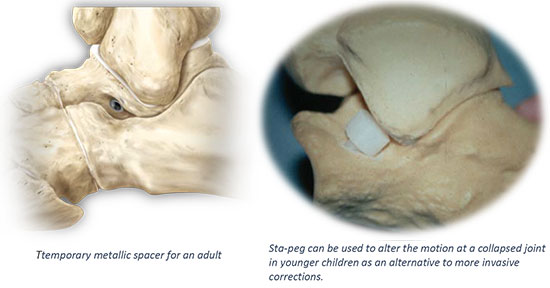
Dr. Perler also occasionally use the sta-peg procedure better for younger patients with flexible flat feet where the bone alignment is still developing so that the foot can adapt to function in a better aligned position.
Joint Repositioning and Fusions

Evans Calcaneal Osteotomy - Lateral Column Lengthening
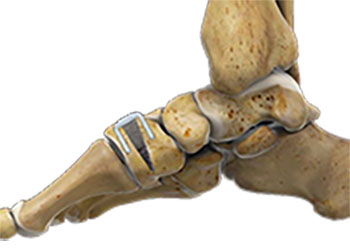
Outward rotation of the foot may occur in patients with flatfoot. An Evans or lateral column lengthening procedure is sometimes performed for these patients. An incision is made on the outside of the foot, and the front half of the heel bone is cut. A bone wedge (typically either titanium or a bone-based graft) is then placed into the cut area of the heel bone. This wedge helps to “lengthen” the heel bone and rotate the foot back into its correct position. The wedge is usually kept in place using screws or a surgical staple.
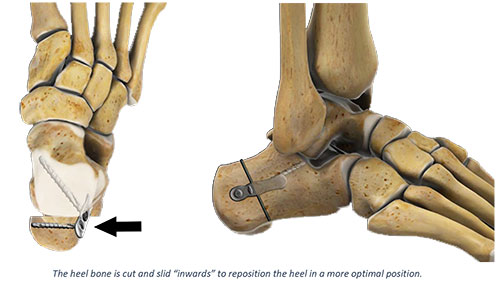
Medializing Calcaneal Osteotomy
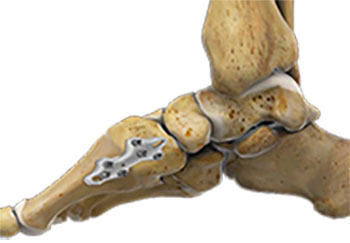
A medializing calcaneal osteotomy (heel slide) procedure is often used when the calcaneus (heel bone) has shifted out from underneath the leg. An incision is made on the outside of the heel, and the back half of the heel bone is cut and slid back underneath the leg. The heel is then fixed in place using metal screws or a plate. This also helps to reposition the Achilles tendon towards the center of the ankle/rearfoot.
Medial Cuneiform Dorsal Opening Wedge Osteotomy (Cotton Osteotomy) or First TarsalMetatarsal Fusion (lapidus)
Arch collapse can lead to the big toe side of the foot being unstable and out of alignment with the rearfoot, allowing the arch to drop more. Your surgeon may perform dorsal opening wedge osteotomy (Cotton) of the medial cuneiform bone to help stabilize the inner arch area. An alternative is to perform a first tarsalmetatarsal joint fusion or Lapidus. Both procedures involve an incision over the top of the foot. In the case of the dorsal opening wedge osteotomy, a bone wedge or titanium graft is placed into the top portion of the bone to push it down toward the floor and stabilize the medial column much like a kickstand on a bike prevents it from falling over. In the case of the fusion, the bone is pushed down toward the floor at the level of a joint in the middle of the foot and the bones are fused into that position. Screws or a plate can be used to keep the wedge in place or to fuse the joint.
Joint Fusions
Arch Joint Fusions
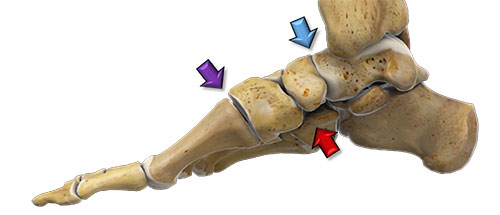
In some cases, other joints of the inner arch may benefit from fusion. This can further help to stabilize the inner arch and prevent recurrence of the condition. Also, in later staged and more advanced flatfoot deformities, one or more of these joints can wear out from abnormal stresses over time which can lead to arthritis. This can include any individual or combination of the following joints; the talo-navicular, the navicular-cuneiform and the first metatarsal-cuneiform joints (see the corresponding colored arrows in the diagram below).
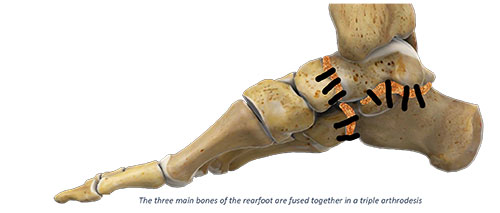
Double or Triple Arthrodesis
In the later stages of flatfoot, deformities are frequently inflexible (stiff). Arthritis of the foot may be present as well. Surgical correction of these severe cases requires fusion of one or more of the foot joints. This procedure is referred to as a subtalar joint fusion, double or triple arthrodesis depending on the number of joints fused.
What happens after surgery?

Patients may go home the day of surgery and very rarely require an overnight hospital stay. The leg will be placed in a splint and should be kept elevated for the first two weeks. Care must be taken to not put any pressure on the backside of the heel. When you are elevating, place a pillow under the calf area and “float” the heel. Also, be sure to ice as directed. Although you will probably not feel the coolness through the dressings, the ice prevents the foot from overheating and keeps the swelling at a minimum. After a couple of weeks sutures are removed if internal ones were not used. A removable boot is then then fitted and dispensed to you. It is important that patients do not put any weight on the corrected foot for 6 to 8 weeks following the operation. Patients may begin bearing weight at 8 weeks (once x-rays confirm the bone healing) and usually progress to full weightbearing by 10 to 12 weeks. For some patients, weightbearing requires additional time. After 12 weeks, patients commonly can transition to wearing a shoe. Inserts and ankle braces are often used. Physical therapy may be recommended.
Potential Complications
Complications may occur with any surgery and are not necessarily your fault, or the fault of your surgeon. Nonetheless, you should understand the risks. Modern surgical approaches typically involve a combination of procedures to realign the bone deformity, lengthen contracted muscles, substitute for the deficient posterior tibial tendon or perform joint fusions. Most modern surgical treatments exceed 85 percent success rate. In addition to standard surgical risks such as infection, blood clots, risks of anesthesia, delayed wound healing, blood clot formation and nerve injury, additional risks may accompany particular procedures. For example, procedures that require bone healing (osteotomy, fusion) can result in a failure to properly heal the bones. The overall complication rates for these procedures are low.
These complications often can be prevented with proper wound care, full patient compliance in regards to weight bearing instructions, and proper rehabilitation. Occasionally, patients may notice some discomfort due to prominent hardware. Removal of hardware can be done at a later time if this is an issue. There is also the possibility of either over or under correction of the deformity. Depending on any residual symptoms, a revision surgery may be required to further optimized your outcome.
Frequently Asked Questions
Will surgical correction of my flatfoot improve the cosmetic appearance of my foot?
Surgical correction of flatfoot is aimed primarily at reducing pain and restoring function. Although surgery will likely improve the cosmetic appearance of the foot, it is not one of the primary goals of treatment.
If I am being treated without surgery, will I have to wear the orthotic or brace for the rest of my life?
Traditionally, it has been thought that orthotics and/or braces will need to be used by a patient for the rest of his or her life. This device serves to supplement for the dysfunctional posterior tibial tendon and help realign the foot. Some studies, though, have suggested that adequate bracing and strengthening may allow the posterior tibial tendon to heal and therefore avoid permanent brace use. This may be the case in select situations.

What kind of activities will I be able to do after surgical correction?
This depends on the type of procedures being performed. Following a successful surgery, you should be able to return to all pre-surgical activities with much less discomfort. If you have undergone extensive bony fusions, you will want to refrain from repetitive high impact activities such as running and jumping. Cycling, swimming, exercise walking, and golfing are all great low impact actives that are suitable for a surgically corrected flatfoot.
If you have any questions about your condition, please do not hesitate to reach out to us to make an appointment so we can review and address any of your concerns.
(727) 547-4700
"So many things are possible just as long as you don't know they're impossible." - Norton Juster, The Phantom Tollbooth

 Flatfoot is a term used to describe a collapsed arch. Medically, the term is
Flatfoot is a term used to describe a collapsed arch. Medically, the term is  If your feet are causing you problems, visit your foot and ankle specialist for an exam. Dr. Perler will take a close look at the structure of your feet and examine how your foot moves and changes shape while sitting, standing, or taking steps. An X-ray can be helpful to understand the severity of the condition. If a tendon or ligament tear is thought to be possible, an MRI may be ordered. In some cases where it Is felt that your flatfoot is not flexible, a CT scan may be helpful in ruling out the joining of two bones that could lead to a reduction of motion (congenital tarsal coalition).
If your feet are causing you problems, visit your foot and ankle specialist for an exam. Dr. Perler will take a close look at the structure of your feet and examine how your foot moves and changes shape while sitting, standing, or taking steps. An X-ray can be helpful to understand the severity of the condition. If a tendon or ligament tear is thought to be possible, an MRI may be ordered. In some cases where it Is felt that your flatfoot is not flexible, a CT scan may be helpful in ruling out the joining of two bones that could lead to a reduction of motion (congenital tarsal coalition).